Treating Achilles Tendinitis Glastonbury
Enjoy Pain-Free Movement
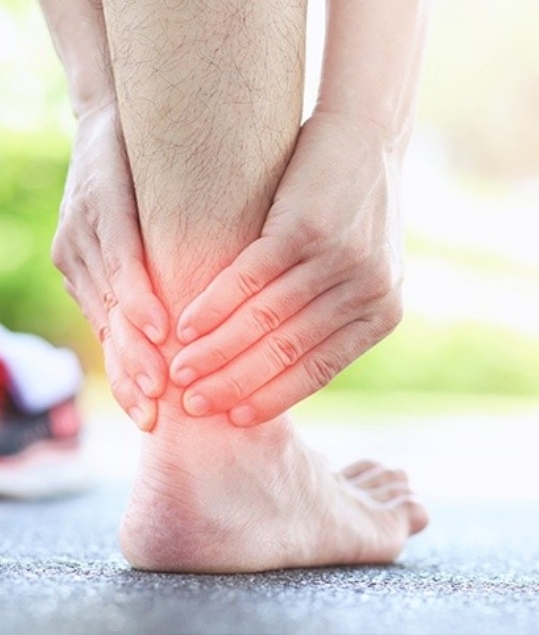
The Achilles tendon is the thick tendon at the back of the heel. It’s formed by the two calf muscles – the deeper soleus muscle and the overlying gastrocnemius muscle, and it’s attached to the back of the heel bone. The primary function of the tendon is to flex the foot. It’s involved in helping you stand up on your tiptoes and propelling you forward when you run. Repetitive overuse or recurring microscopic tears are the most common causes of Achilles tendinitis. Sometimes in severe cases, the tendon completely ruptures, in which case surgery needs to be considered. Keep reading to learn more about how our team here at the New England Stem Cell Institute uses regenerative medicine to assist with Achilles tendinitis in Glastonbury.
What are the Symptoms of Achilles Tendinitis?

Symptoms of Achilles tendinitis include pain and/or stiffness in the Achilles tendon during or after an activity, inflammation or swelling of the tendon, nodule formation in the tendon (which looks like a marble stuck in the middle of the tendon), and tenderness when squeezing the tendon.
How is Achilles Tendinitis Diagnosed?

Diagnosing Achilles tendinitis usually is straightforward. In most cases, a physical exam is all that’s needed to confirm the diagnosis. Diagnostic ultrasound can also be helpful to identify any tears within the tendon.
How is Achilles Tendinitis Treated?
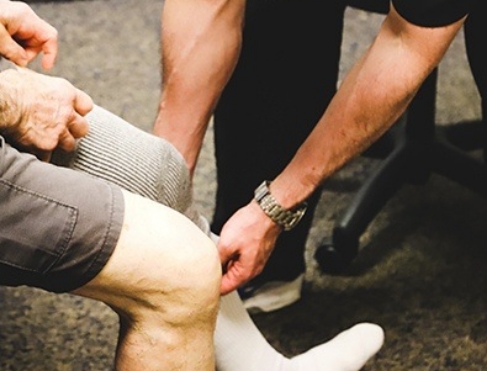
Treatment for Achilles tendinitis starts with conservative approaches including physical therapy, cold/hot compresses, heel cups/lifts (to reduce the tension on the tendon), night splints, and stretching/strengthening exercises. When these conservative measures fail, the TenJet® treatment may be helpful.
Certain types of nerve blocks can also be helpful in reducing or alleviating pain and promoting tendon healing and repair. But when all of these conventional approaches don’t help, then regenerative medicine treatments such as prolotherapy, PRP, and other orthobiologics may be the answer. These treatments take advantage of the body’s natural healing mechanisms to repair the tendon and relieve symptoms.
